Facing COVID-19, a series of Council on Criminal Justice web events, features leaders on the front lines of protecting public safety, public health, and justice as the criminal justice system responds to the coronavirus pandemic. COVID-19 and Corrections: Challenges and Strategies took place on April 30, 2020.
Featured Speakers
Sheriff Ed Gonzalez – Harris County, Texas
Colette Peters -Director, Oregon Department of Corrections
Anne Precythe – Director, Missouri Department of Corrections
Louis Reed – National Organizer, #cut50
John Tilley (moderator) – CCJ Senior Fellow, attorney, five-term state legislator, and former Kentucky Justice Cabinet Secretary
Summary
People behind bars are especially vulnerable to COVID-19. Leaders who run correctional facilities say they are using medical guidance, targeted testing, housing modifications, and other tools to keep incarcerated populations – and staff who oversee them – safe from infection.
Speaking at a Council on Criminal Justice (CCJ) web conference on corrections and COVID-19, leaders of three corrections systems acknowledged the challenges of limiting the spread of the virus inside prisons and jails but said their strategies had so far prevented major, deadly outbreaks.
“It has been all about planning,” said Oregon Department of Corrections Director Colette Peters, a member of CCJ’s Board of Trustees. She added, however, that while the state’s prisons have seen low infection numbers so far, “it can all change tomorrow.”
Louis Reed, a CCJ Board of Trustees member and national organizer for the advocacy group #cut50, urged elected officials to reduce risk inside jails and prisons by freeing people over 65 and those within six months of their scheduled release date.
“Now is the time for bold ideas, for questioning how we do business,” said Reed, who spent nearly 14 years in federal prison.
Sheriff Ed Gonzalez agreed, noting that he had sought authority from local leaders to carry out “compassionate release” on a broad scale to thin the Harris County Jail population, but had lost that bid.
Instead, Gonzalez has worked with judges and other stakeholders to reduce the population more incrementally, even as the number of jailed people awaiting transfers to state prison grows because new admissions are on hold.
“We can’t check humanity at the door,” Gonzalez said. “We’re all in this together.”
The video conference was the third in a series hosted by CCJ and designed to explore the impacts of COVID-19 on criminal justice and how leaders are coping with the changed landscape. Held on April 30, the conference on corrections drew more than 700 registrants.
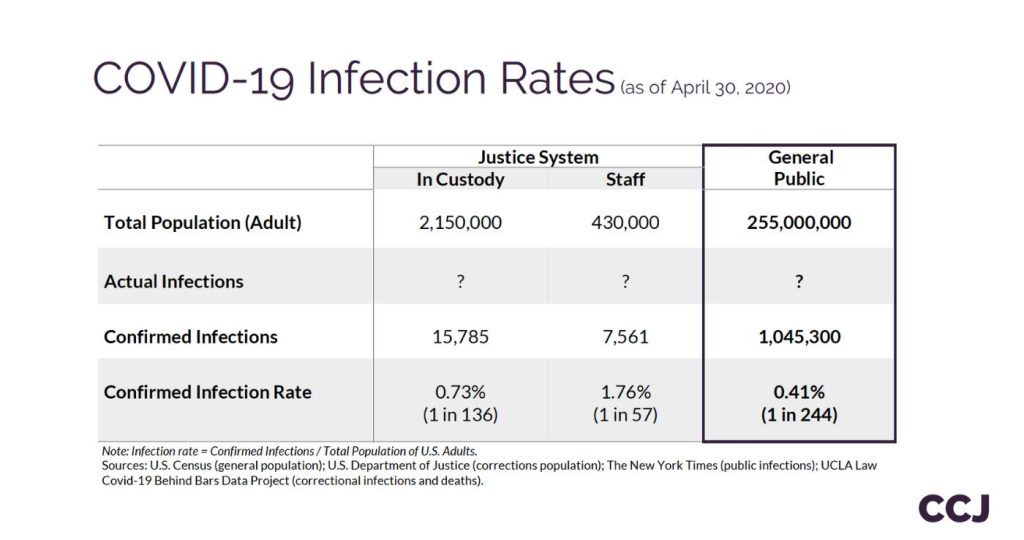
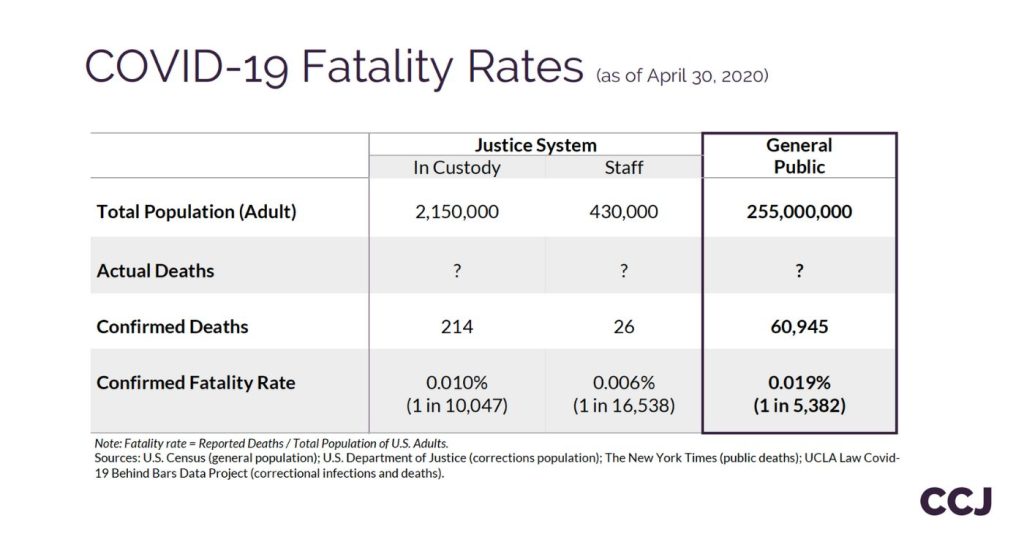
Key Takeaways
Using Quarantines, Housing Modifications to Limit Infection
Prisons and jails have limited space, and incarcerated individuals – especially those in dormitory style housing units – typically have little ability to practice social distancing. Corrections administrators are managing by quickly separating symptomatic people and others in their living area from the rest of the incarcerated population, and using targeted follow-up testing to assess the effectiveness of such moves. Some facilities also are quarantining newly admitted individuals to minimize the possible spread of the virus.
GONZALEZ: “We’ve taken steps to quarantine people upon booking at the front end, and then in the jail, we’ve quickly separated individuals when they’ve become symptomatic. When someone tests positive in a cellblock, we find that the rest of cellblock usually tests positive at a rate of about 70%. So we’re taking individuals who are symptomatic, removing them, and quarantining the rest of the cellblock. It’s a lot of moving parts, but we believe that monitoring in real time, and using that testing data to drive our decision-making, is providing good results. We’ve only had four individuals hospitalized to date.”
PETERS: “Our team at intake re-envisioned and reimagined what it would mean to accept people from the community who might be positive. We have not had a positive test come through yet at intake, which is fantastic, but we have set up a quarantine system for those individuals who are coming in so that they are separated from the rest of the population for 14 days before they move further into our institutions. We also do medical screening daily. So far so good.”
PRECYTHE: “From the beginning, we’ve followed an aggressive viral containment plan. As soon as we had the first symptomatic person we quarantined the entire wing of that person’s housing unit. We later did screenings of the other three wings and found no positives in those wings, and no people who were symptomatic. So we feel very confident about our viral containment plan.”
Visitation Restrictions, Personal Cleaning Products, Other Tools Help Contain Spread
While social distancing is a key preventive measure in the free world, it can be a challenge behind bars, especially in crowded living units. Corrections officials have increased disinfecting regimens, distributed extra soap, and made various operational changes. All 50 states, for example, have imposed some limitations on visitation, with 15 states suspending all visits.
PETERS: “Our governor locked down the state immediately at the beginning of March and we were able to do that inside our institutions as well. While it was incredibly difficult to make that decision to stop volunteers, visitors, and contractors from coming into our institutions, I think that was our [most effective] social distancing measure in Oregon.”
PRECYTHE: “In Missouri we made sure that we had enough sanitizer available in the housing units as well as on the ground in our institutions for staff and for the offender population, and that they had enough soap. I sent a message to our offender population asking them to practice social distancing, wash hands frequently, and clean their areas. How can you ask someone to take care of themselves and then not provide them with what they need to do that?”
REED: “We need to make sure hand sanitizer stations and other personal hygiene products are available to people who are incarcerated free of charge. As someone who did almost 14 years in federal prison, I think it’s absolutely asinine that in New York, you have incarcerated people produce hand sanitizer that the incarcerated population can’t even use because [it contains alcohol and] it’s considered contraband. We also need to suspend co-pays for medical visits for people who are incarcerated.”
The Case for–and Against–Expedited Releases
Since COVID-19 surfaced, advocates, attorneys, and relatives of incarcerated people have pressed authorities to release large numbers of individuals in custody – especially those who are elderly or have underlying health conditions. Some jurisdictions have authorized expedited releases, while others have not altered their policies – and maintain that certain individuals could face greater vulnerability in the community.
GONZALEZ: “When this pandemic started, our jail population was hovering around 9,000 individuals, and about 70% are typically pretrial detainees. Now we are at about 7,500. Early on, we tried to advocate aggressively for compassionate release, talking to different decision makers, but a broad, mass release up front wasn’t to be. So instead, we armed our judges with data in terms of risk factors and other things to help them make the best decisions, and we feel those efforts have paid off over time, as we’ve seen a decline in our population incrementally.”
PETERS: “We’ve had substantial conversations around early release … and the governor made a decision not to move in that direction because this is very complicated. Counties are shut down right now, and community resources are very limited. We are still releasing 400 individuals every month based on our normal numbers, and we barely have resources for them. So for Oregon, I think it would be a misstep to push people into the community in a mass release without resources and medical services to help support them. I don’t like to think of a prison system as a social services system, but in the midst of a pandemic, we have 15,000 individuals [in custody] who have three meals a day, a roof over their head, and access to quality medical care.”
REED: “I have never had a conversation with any incarcerated person who said, ‘Hey, I’m at risk of infection, but I don’t want to be released, I don’t want to get back to my family, I don’t want to get back to my community because of a lack of resources.’ We need to identify people who are scheduled to be released from prisons and jails within the next six months and we need to get them out and into home confinement, barring a specific reason not to do so. Second, we need to parole people who are over the age of 65, with priority given to those with underlying health conditions that make them particularly susceptible to the virus.”
Medical Advice, Testing, Other Data Drive Decision-Making
Correctional administrators are leaning hard on public health authorities, a partnership that, in many cases, was not well developed before COVID-19. The medical guidance has been an invaluable weapon in the fight to contain the virus behind bars.
PETERS: “We’re very fortunate because our medical team is connected at the hip with the Oregon Health Authority and their epidemiologists. Every decision we’ve made has been based on medical advice and direction, along with the CDC standards.”
GONZALEZ: “Our medical team has been phenomenal. Every day we poke holes in our plan, we take a holistic approach. Our medical team, our correctional team, and support personnel are all on our daily calls. We’ve tested over 650 individuals in our jail population, and at the moment we have 392 who have tested positive. We’ve had no loss of life with our personnel nor with our inmate population, so that’s key.”
PRECYTHE: “From the beginning, our staff have taken very seriously the precautions laid out by the CDC and our Department of Health and Senior Services, and we’ve been able to do screening and temperature testing when anyone comes into our facilities. If anything good comes out of this pandemic, it’s the awareness of how much the institutional community needs its public health department.”
REED: “If we had other corrections directors around the nation following the lead of Director Peters and Precythe, and Sheriff Gonzales, we’d be much better off with our institutions in terms of preventing infection and death … I applaud the efforts of the dedicated men and women in uniform doing their best to show up day in and day out, to make sure people on the inside are protected. But we have to do more.”
Addressing Fear, Inside and Outside the Walls
The threat of COVID-19, along with the many unknowns related to the coronavirus that causes it, has sparked fear across the nation. For incarcerated people, that anxiety can be compounded by a lack of information and sense of powerlessness. Meanwhile, community members in some areas have expressed safety concerns about expedited releases and the return of formerly incarcerated people who may have tested positive for the virus.
PETERS: “We are all in a state of heightened alert, worried about what this virus will do to our families, our friends, our loved ones, and the same is true for those who are incarcerated. That fear factor is high. And we need help convincing the community that individuals who are incarcerated were part of their community before they went to prison, and they’re certainly part of their community now as we transition them out. I have concerns that this fear factor could turn into a bit of a scarlet letter for these individuals who are releasing, especially those releasing from facilities where we have had positives.”
REED: “I am in contact with more than 360 incarcerated individuals nationwide, people on the federal level, on the state level, on the local level, and they are reporting to me, day in and day out, ‘Louis, I am going to die in here.’ Irrespective of whether you wear brown or you wear blue, this virus doesn’t discriminate. We’re talking about human lives. We’re talking about mothers, fathers, sisters, brothers, people who will eventually make up the fabric of our community. We need to make sure they are safe, and that they come out better and healthier than when they went in.”
GONZALEZ: “When I became Sheriff three years ago, 90,000 children in our county had a parent incarcerated in my jail each year. We’re having a food drive focused on those families who have someone incarcerated, and we’ve received a very positive reaction from people incarcerated because they see we’re taking care of their families. We’re trying to think beyond the four walls of the jail cell during this unprecedented time.”
The Importance of Communication and Transparency
Keeping the public – and people behind bars – informed of infection rates and measures used to reduce risk behind bars is a key strategy employed by correctional administrators. Transparency can help build trust, inside and outside the walls.
GONZALEZ: “Providing transparency has helped assure our community that we are running a good operation, that we are following science and data. Every day we release our numbers [of infections], and I think we’ve been able to build some strong capital with our community. Before COVID-19, we created a public dashboard so the public can see what our daily population looks like.”
PRECYTHE: “Another thing that has been important is how we’ve communicated to the offender population. We want to make sure they understand that the things we are doing are things we are doing for them, not to them, and that we are in this together, staff and the offender population. This virus does not distinguish one or the other.”
REED: “This is not a matter of our heads, it’s a matter of our hearts. And ultimately, over time, our values are going to be interrogated, they are going to be prosecuted, and they will be evaluated by how we responded to the so-called least of us.”
Taking Care of Staff
GONZALEZ: “We know anxiety is high. I have over 192 personnel at our jail who are currently infected. We know that affects their colleagues, but they are still showing up for work. We are doing equipment drives for them to make sure their families are taken care of, and every day our communications team puts out a newsletter to our staff. So often we communicate to all other stakeholders but not our own. We want them to know in real time what’s going on, how we’re addressing challenges, and about opportunities for mental health support so they can get the help they need.”
PETERS: “In terms of the community mindset, we have had some negative reactions to some of our staff, while in uniform, shopping at the grocery store and maintaining social distancing. It was related to the fact that they worked at a facility that had some positive testing. I would love to see a call to action to reach out to those correctional professionals and help the community understand that they are first responders, they are essential personnel during this pandemic, and they need to be treated with compassion and be supported now more than ever.”


